 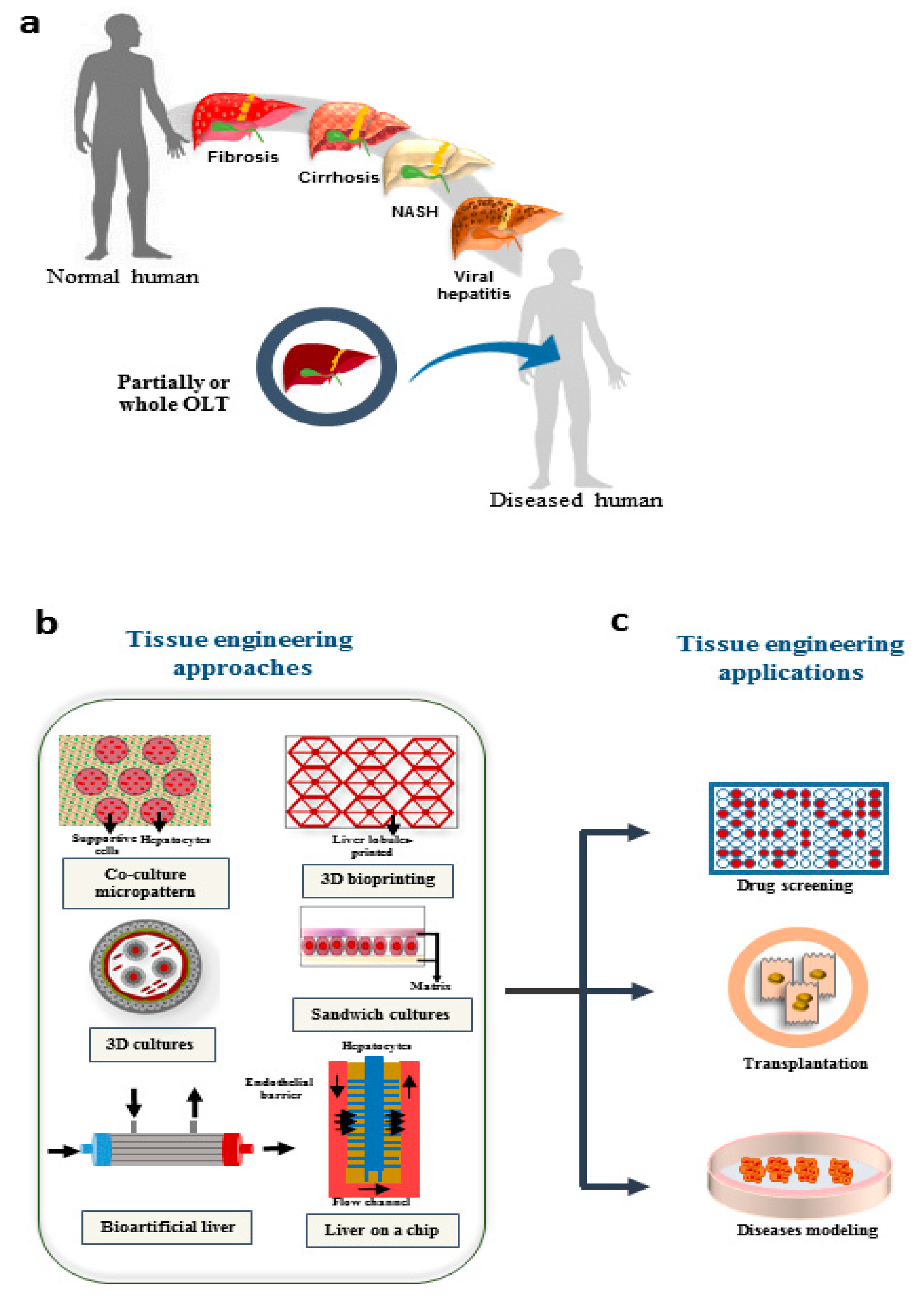 
Therefore, due to the aforementioned limitations, alternative therapeutic approaches are necessary to bridge or replace affected organ. The OLT faces several limitations and obstacles including the shortage of donated organs, post-operational complications and high hospitalization costs as well as the need for a life-long immunosuppressive therapy. Orthotopic liver transplantation (OLT) is the “gold standard” and the only established treatment for end-stage liver diseases and acute liver failure. Such ability can be significantly impaired when the liver faces a severe acute injury or an extreme chronic disorder which is commonly associated with progressive liver inflammation and fibrosis. A healthy liver shows excellent regenerative capacity in response to injury. An active, efficient interaction between hepatocytes and the surrounding cells and/or microenvironment is necessary for their maintenance and proper function. Hepatocytes are liver parenchymal cells, while cholangiocytes, endothelial cells, tissue-resident macrophages (Kupffer cells), and stellate cells are known as the liver non-parenchymal cells. 
Among liver disorders, nonalcoholic steatohepatitis (NASH) and cirrhosis are common. According to world health organization (WHO) reports, liver diseases are the 12th cause of mortality globally and their incidence and prevalence are increasing. In this regard, failure of liver functions may lead to a wide range of liver dysfunction conditions with different levels of severity, morbidity or mortality. The liver plays a crucial role in different physiological functions such as protein, carbohydrate, and lipid metabolism, detoxification of xenobiotics, storage of glycogen and vital biomolecules, production and excretion of bile and cholesterol compounds, synthesis of albumin and clotting factors, ammonia detoxification and more. Herein, we summarized novel technologies used in liver regenerative medicine and their future applications in clinical settings. Taken together, new findings indicated that developing liver tissue engineering-based techniques could pave the way for better treatment of liver-related disorders. Common TE techniques are based on allocating stem cell-derived hepatocyte-like cells or primary hepatocytes within a three-dimensional structure which leads to the improvement of their survival rate and functional phenotype. In this regard, a variety of techniques (e.g., fabrication technologies, cell-based technologies, microfluidic systems and, extracorporeal liver devices) could be applied in tissue engineering in liver regenerative medicine. Liver tissue engineering (TE) enables us to reproduce and restore liver functions, fully or partially, which could be used in the treatment of acute or chronic liver disorders and/or generate an appropriate functional organ which can be transplanted or employed as an extracorporeal device. In the context of emerging regenerative medicine, researchers are trying to regenerate and replace different organs and tissues such as the liver, heart, skin, and kidney. Organ and tissue shortage are known as a crucially important public health problem as unfortunately a small percentage of patients receive transplants. 
0 Comments
Leave a Reply. |

 RSS Feed
RSS Feed
